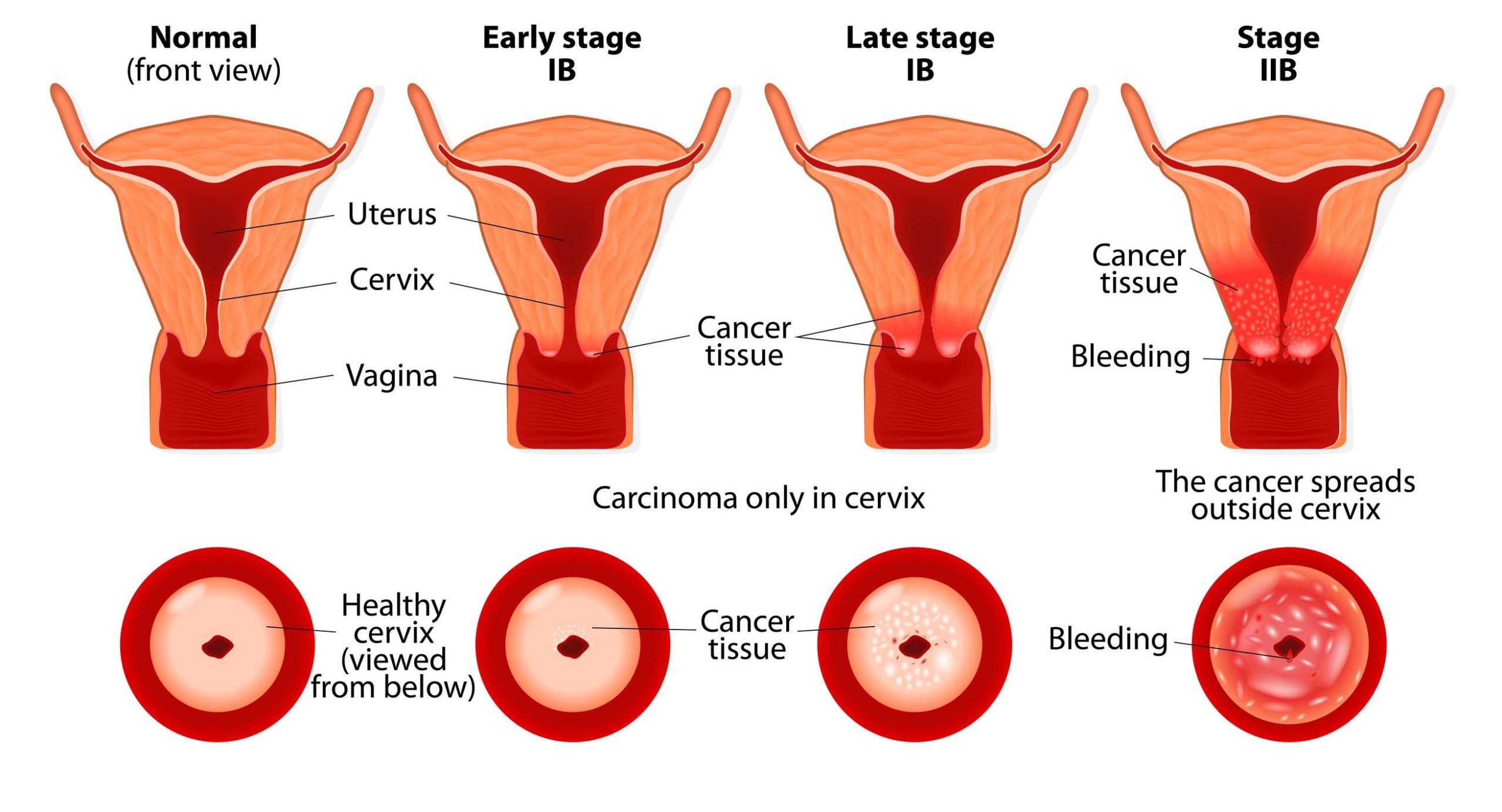
Conization is necessary when a patient’s cervical screening (or commonly known as a Pap smear test) results come back as abnormal. When this happens it is important to surgically remove the affected cervical tissue to prevent the development of cervical cancer.
Conization is used both as a diagnostic tool and treatment: tumors, pre-cancerous conditions and inflammation can be diagnosed and also treated with conization.