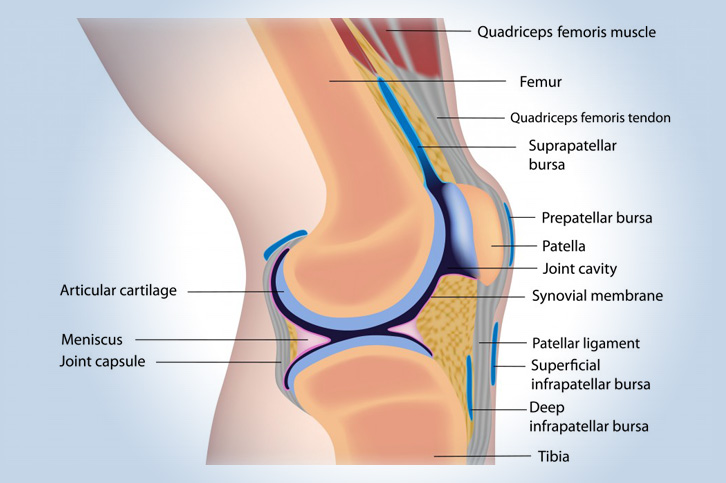
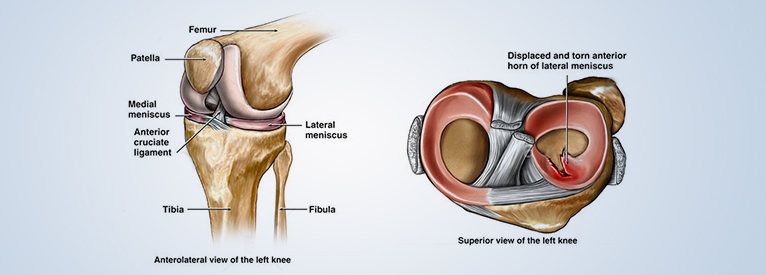
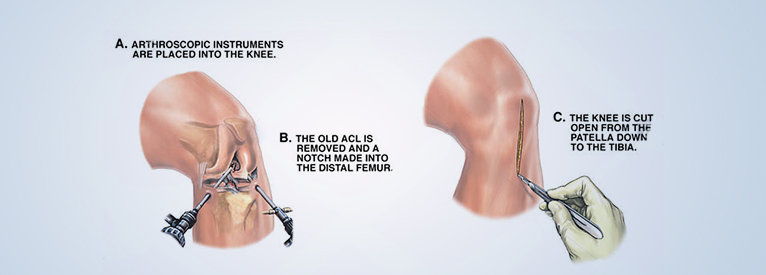
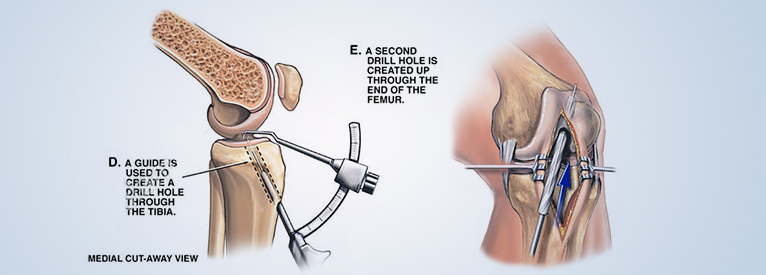
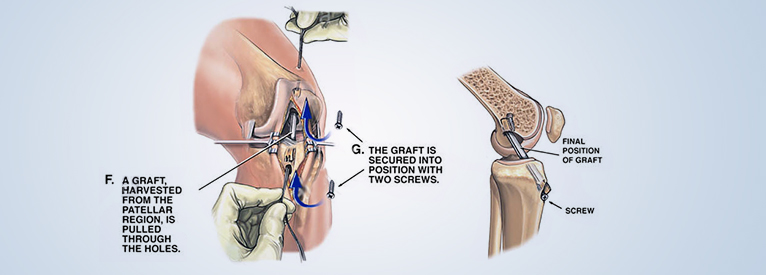
The knee is one of the largest and most complex joints of the human body. The knee connects the thigh bone (femur) to the shin bone (tibia). There is a smaller bone that runs alongside the tibia called fibula, and the kneecap (or patella) is the fourth bone that makes the knee joint. Tendons attach the leg muscles that move the knee joint to the knee bones. Ligaments join the knee bones and provide stability to the knee:
- The anterior cruciate ligament prevents the femur from sliding backward on the tibia (or the tibia sliding forward on the femur).
- The posterior cruciate ligament prevents the femur from sliding forward on the tibia (or the tibia from sliding backward on the femur).
- The medial and lateral collateral ligaments prevent the femur from sliding side to side.