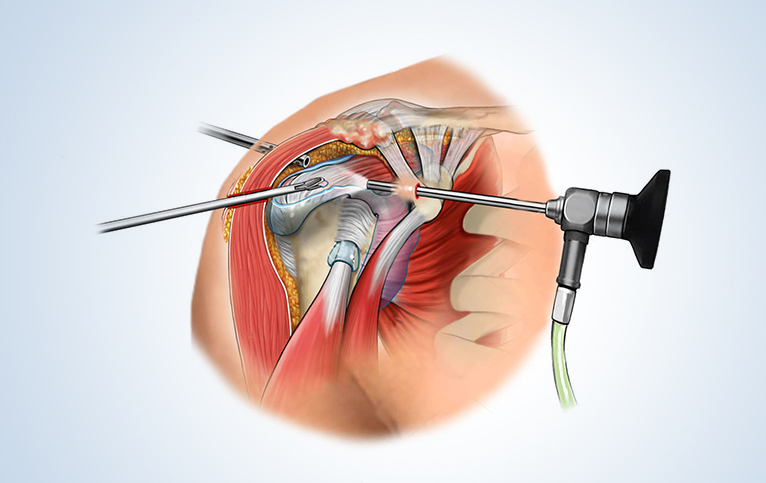
The shoulder is the most complex and unstable joint in the body and it can get injured easily. Your shoulder joint is composed of three bones: the clavicle (collarbone), the scapula (shoulder blade), and the humerus (upper arm bone). Your shoulders are the most movable joints in your body.
- Safety First COVID-19
-
Treatments
-
Orthopaedic Surgery
- Arthroscopic knee surgery
- Arthroscopic meniscectomy
- Anterior cruciate ligament (ACL) surgery
- Bunion surgery
- Carpal tunnel release
- Chondropathy surgery
- Cubital tunnel release
- Dupuytren’s contracture surgery
- Ganglion Removal
- Hammertoe surgery
- Hip replacement surgery
- Laser Disc Decompression (PLDD)
- Patellar dislocation
- Shoulder surgery
- Total knee replacement
- General Surgery
- Hand surgery
- Gynecological surgery
- ENT Surgery
- Ophthalmic Surgery
- Diagnostics
- Urological surgery
- Proctology
-
Orthopaedic Surgery
- Prices
- Our hospital
- Our Team
- Travel Guide
- Blog
- Contact